In Brief:
- Currently, 119,000 Americans are on the national transplant waiting list
- Organ donors and recipients must be “matched” before a transplant
- Antibody testing may allow for more successful transplants
In a world as fast-paced as ours, simply waiting in a long line at the supermarket can feel like a death sentence. Imagine if, instead of a line at the store, you were on an endless waiting list for an organ transplant you desperately needed. Currently, 119,000 people are on the national transplant waiting list with another name added every 10 minutes. While we may groan about supermarket lines or stalling traffic, for these 119,000 Americans, waiting really can be a death sentence.
However, researchers like Dr. Prakash Rao stand defiantly in the face of stalling science and ask, “what’s the holdup?” Dr. Rao is the Vice President of Diagnostics & Research Operations and the Director of the Transplant Laboratory at the NJ Sharing Network, a non-profit organization for organ recovery and placement. He and other researchers from the NJ Sharing Network are working to change the grim reality of the transplant waiting list by making the organ matching process more efficient.
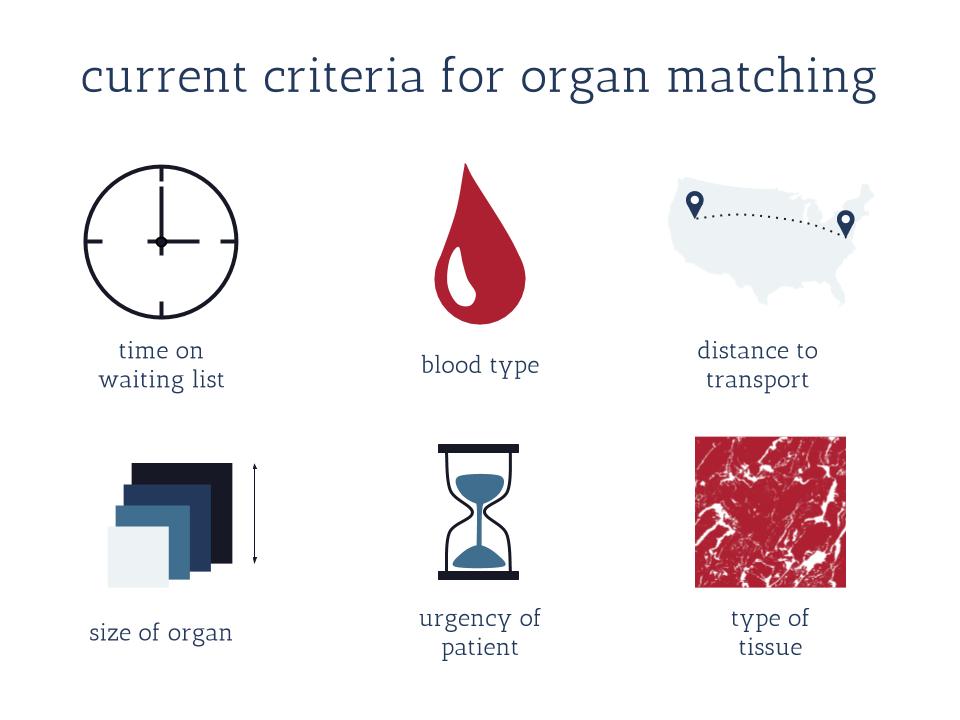
The matching process between potential organ donors and recipients is a lot like dating. The organ donor and recipient must be compatible, otherwise, the recipient’s body will reject the donor’s organ. First, individuals are selected based on various criteria such as blood type, tissue type, and medical urgency of the patient. Once all these factors align, a final test called a crossmatch is performed. In this “transplant in a test tube,” as Dr. Rao calls it, samples of the donor and recipient’s blood are mixed to see if the recipient’s antibodies will attack the donor’s cells. Antibodies are immune cells that act like soldiers that defend our bodies against harmful foreign invaders. If the recipient’s antibodies are likely to attack, then the transplant will not be successful.
Dr. Rao is currently researching a way to make the match process more specific so that transplants can occur even when the crossmatch results predict rejection. He believes that although the test may indicate ominous recipient-donor interactions, certain antibodies will not attack. Dr. Rao works specifically with Immunoglobulin G or IgG antibodies. There are four subtypes of IgG antibodies — IgG1, IgG2, IgG3, and IgG4 — out of which only IgG1 and IgG3 attack foreign cells, while IgG2 and IgG4 usually do not. Essentially, IgG2 and IgG4 are soldiers on guard that never make a move. Therefore, if only IgG2 and IgG4 antibodies are present, transplants can still occur.
Dr. Rao and his team are working tirelessly to define a specific test that determines which antibodies are present in a patient’s blood sample. If they succeed, about 10,000 more transplants can be carried out per year.
We can rest assured that Dr. Rao will not give up. Waking up at 2:30 a.m. every day, he quotes Robert Frost with great pride: “The woods are lovely, dark and deep, but I have promises to keep. And lives to save before I sleep.” With his research and perseverance, Dr. Rao’s work will likely save thousands of lives. Although those on the transplant list must wait for now, they are not without hope. After all, Dr. Rao’s not waiting around.
Works Cited
- “Organ Donation Statistics.” Organ Donation Statistics: Why be an Organ Donor?
Accessed August 20, 2016.
https://organdonor.gov/statistics-stories/statistics. html#glance. - “Organ Procurement and Transplantation Network.” Learn about the Donor Matching
System – OPTN. Accessed August 20, 2016.
https://optn.transplant.hrsa.gov/learn/about- transplantation/donor- matching-system/. - Dr. Prakash Rao, Ph.D., MBA, FACHE, HCLD (Vice President of Diagnostics &
Research Operations and Director of Transplant Laboratory) in discussion with the
author, August 2016.
Image Credits:
Feature Image:
Graphic by Staff Illustrator, Aparna Kumar
Story Image:
Graphic by Staff illustrator, Selena Liu
- “Flag map of the contiguous United States https://commons.m.wikimedia.
org/wiki/File:Flag_map_of_the_ contiguous_United_States_( 1912-1959).png” by Anonymous https://commons.m.wikimedia. org/wiki/User:DrRandomFactor (Edited). License: CC BY-SA 3.0 - “Marble Pattern https://commons.m.wikimedia.
org/wiki/File:Marble_pattern_ 008.jpg” by Anonymous (Edited). License: CC BY 3.0
Chief Editor: Aparna Ragupathi
Creative Team Coordinator: Sreya Das
Team Editor: Manasa Gadiraju
Team Graphic Designer: Aparna Kumar
This article was written by Varsha Garla. As always, before leaving a response to this article please view our Rules of Conduct. Thanks! -cSw Editorial Staff